Pride Yourself on Your Health

This summer, take a few moments to focus on the most important woman in your life. You. Dr. Anita Radix addresses some pressing lesbian health issues.
”I was recently diagnosed with HPV. I’ve only ever had sex with women, and I thought I couldn’t get a sexually transmitted infection (STI), but obviously I thought wrong. Are there other STIs lesbians are susceptible to? And how do I ensure I don’t spread this to future sexual partners?”
In the last few years several studies have shown that up to 13% of lesbians are infected with the Human Papillomavirus (HPV). There are many types of HPV, some of which cause genital warts and others that may lead to abnormal cell changes on the cervix, causing cervical cancer if left untreated.
Cervical HPV infection may even be found in women who have never had a male partner. If you never had a male partner yourself, chances are that had a girlfriend who has, and who may be infected.
HPV can be transmitted from person to person through direct skin-to-skin contact, not excluding vaginal and anal sex. A woman who has HPV can also transmit it to her female partner through fingeringand sharing sex toys. In general, lesbians are at decreased risk for STIs compared with the general population, however all STIs, including herpes, chlamydia, gonorrhea and syphilis can be transmitted between female partners.
Using dental dams, not sharing sex toys, cleaning toys between partners and using condoms may be helpful in preventing the spread of some STIs, though it is not known if this can always prevent the transmission of HPV.
The most important lesson for lesbians is to know that they are at risk for HPV infection and cervical cancer. All women aged 18 and older (younger, if sexually active) need to have regular Pap smear screenings. If detected early, cervical changes can be treated before cancer develops.
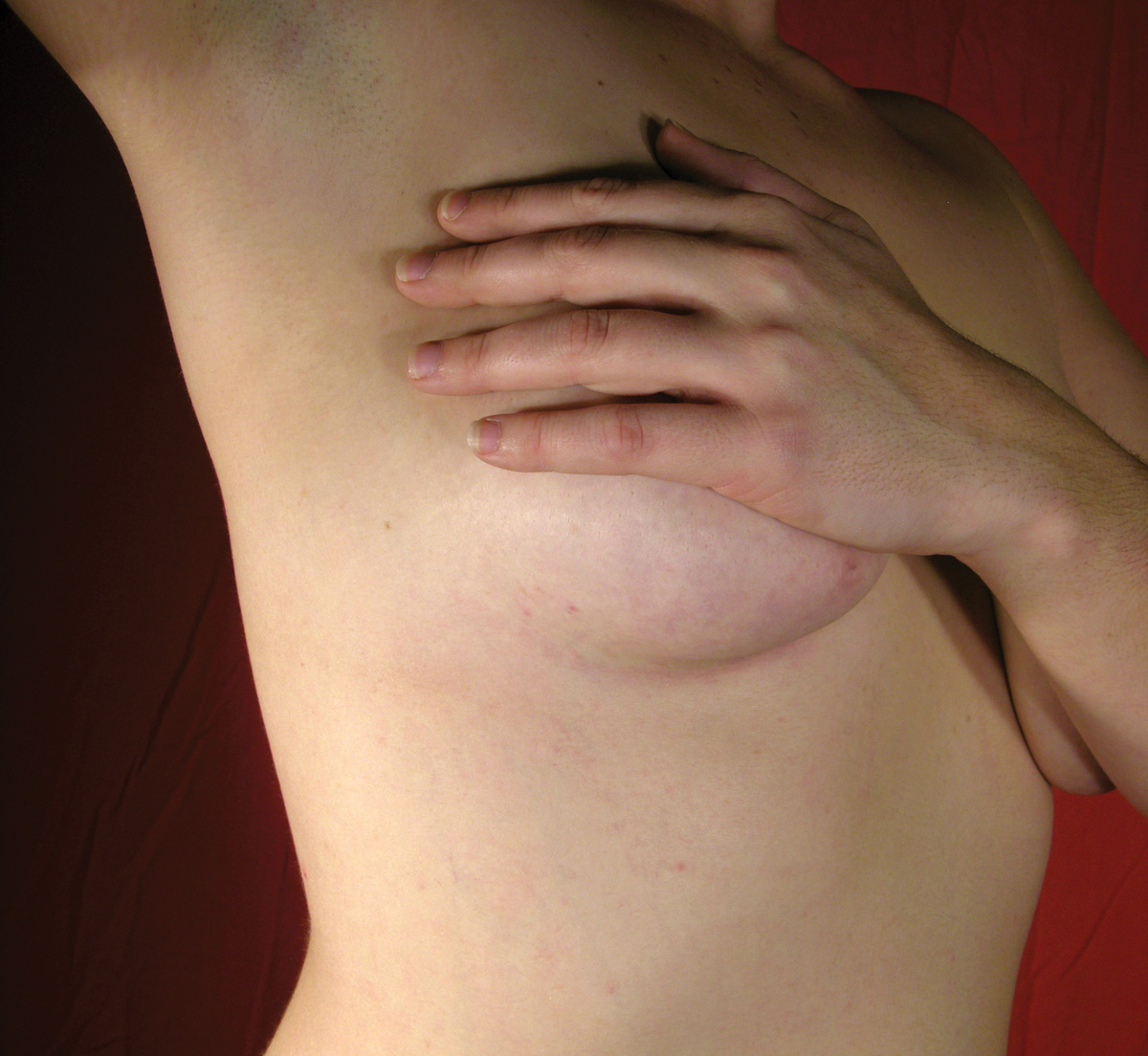
“I heard that lesbians are more likely to get breast cancer than other women. Is that true?”
All women, regardless of their sexual orientation, should be aware of breast cancer risk. Breast cancer is the leading cause of cancer in women—about 1 in 8 women will develop breast cancer during their lifetime.
There are several factors that can increase a woman’s chances of a breast cancer diagnosis. As women age, their risk increases, which is why regular mammography is encouraged in women over 40. Other women who are at risk include those who delay childbirth until after age 30, those who have a close family member (mother, sister) with breast cancer, early onset of menstruation and those who are overweight. Lesbians as a group may be at higher risk for breast cancer than non-lesbian women because they are less likely to have children or delay having children until after age 30.
It is very important to understand that many women with breast cancer have no clear risk factors, and that is why it is so important for all women to be involved in early breast cancer detection. When breast cancer is detected in the early stages, the options for treatment and cure are greater.
The American Cancer Society Guidelines for the Early Detection of Cancer recommend that women begin yearly mammograms at age 40. Clinical breast exams (CBEs) should be given by a medical provider at least every 3 years for women in their 20s and 30s and yearly after age 40. If you are doing monthly breast self-exams, recommended after age 20, it is important that you contact your medical provider if you detect a lump.
One of the reasons that lesbians may not participate in regular breast cancer screenings is because of financial concerns. In New York State, there is a program aimed to provide lower-income women with free Pap smear screenings, CBEs, and mammograms. To find out more information about the Breast and Cervical Cancer Detection EducationProgram, visit health.state.ny.us, keyword: Cancer Services, to find a partnership near you.
“I think I might be transgender. A transitioning friend of mine uses testosterone, and I’m thinking of trying it to find out if it feels right. But I’m worried that there could be some negative side effects. Is it safe to take T? Should I get a prescription first?”
Transitioning from female to male on testosterone (T) can be very safe and dramatically effective. Thousands of transguys have used T to change their physical appearance to a masculine one with few or no side effects. However, you are right to be concerned about possible side effects. I recommend that every transgender person who chooses to use hormones do so under an experienced medical provider’s supervision. Beginning cross-gender hormone therapy is an important decision and should only be done after you are aware of all the possible effects, both positive and negative. Using T may sometimes lead to medical problems such as liver disease, diabetes mellitus (high blood sugar), high cholesterol and high blood pressure. T may also be linked to polycystic ovary disease and cancers of the breast and uterus.
I would recommend first joining a trans support group. If you decide to begin taking hormones, even as an experiment, it is important to see a medical provider who has training in transgender health care.
The medical provider will first take a complete history, perform a physical exam and run laboratory tests to screen for any medical problems that could make taking T more dangerous. In addition, since transition can be difficult both physically and mentally, it is always a good idea to have the support of a trangender-experienced therapist or counsellor while taking hormones. You will also be given advice on how to reduce complications while on T by not smoking, reducing alcohol and drug use, and following a healthy diet and exercise program. After starting hormone therapy, you will need to be monitored on a regular basis to check for side effects. Your medical provider will routinely perform laboratory tests for liver function, lipids (cholesterol) and blood sugar. The dose of testosterone can be adjusted upwards for more masculinizing effects or downwards to reduce the risk of complications, depending on an individual patient’s needs.
As you can see, taking hormones without a prescription and without being monitored carefully can be risky. Of course it may sometimes be difficult to find a medical provider who is trans-sensitive and well versed in cross-gender hormone therapy. In the New York City area, contact the LGBT Community Center (gaycenter.org) and the Callen-Lorde Community Health Center (callen-lorde.org) for more information on providers.
Anita Radix MD MPH, associate medical director of the Callen-Lorde Community Health Center, answers your questions about