States Across The Country Are Restricting HIV Treatment Programs
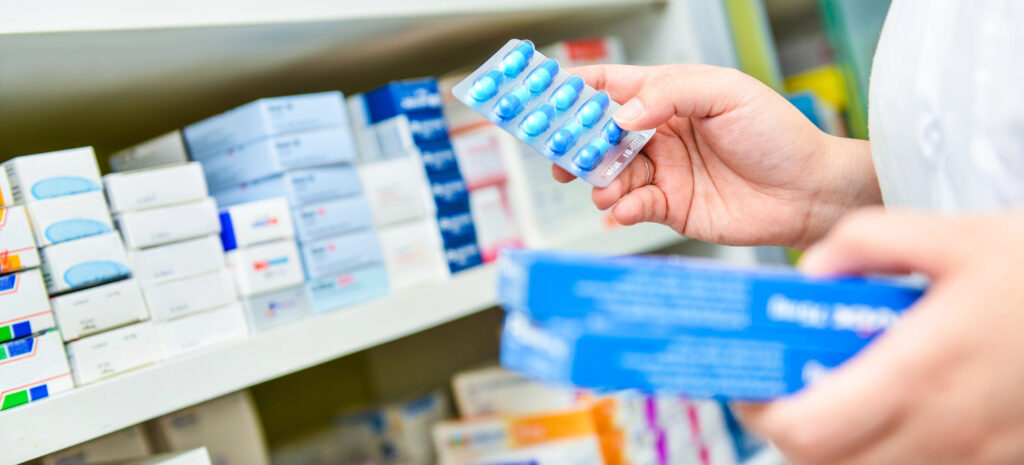
As costs rise and funding stalls, more states are cutting or limiting programs that help thousands of Americans afford HIV treatment.
Featured image by MJ_Prototype via Getty
Thousands of people living with HIV are facing new uncertainty about their access to lifesaving medication as states tighten rules for programs that help cover treatment.
Nearly 20 states have implemented or are considering restrictions on AIDS Drug Assistance Programs, known as ADAPs, according to recent analyses from public health researchers and advocacy organizations. The programs help people living with HIV pay for medications or insurance premiums, ensuring they can maintain consistent treatment.
For many patients, ADAP serves as a critical safety net. Roughly 25 percent of the estimated 1.2 million people living with HIV in the United States rely on the program for some form of medication or insurance support.
The growing restrictions are largely driven by financial pressure. According to the February 2026 ADAP Watch report from the National Association of State and Territorial AIDS Directors, federal funding for the programs has “remained relatively unchanged over the last decade,” even as enrollment and healthcare costs have climbed.
Related: Protesters Arrested For Demanding Release of Billions in Life-Saving HIV/AIDS Funding
Enrollment in ADAP programs surged about 30 percent between 2022 and 2024, in part because many people were removed from Medicaid coverage after pandemic-era protections ended. At the same time, the cost of HIV medications and insurance premiums has continued to rise.
“Effectively, programs are being asked to do more with less federal funding,” Lindsey Dawson, associate director of H.I.V. policy at KFF, told the New York Times.
In response, at least 18 states have adopted cost containment measures. Some have lowered income eligibility thresholds, meaning people who once qualified for assistance may no longer be eligible. Others have reduced the number of medications covered or tightened documentation and recertification requirements.
Pennsylvania, for example, lowered eligibility from 500 percent to 350 percent of the federal poverty level, affecting roughly 1,600 people. Kansas has reduced eligibility for premium assistance from 400 percent to 250 percent of the federal poverty level, while Delaware and Rhode Island have also reduced income limits.
Public health experts warn that more states may adopt similar measures as budgets tighten and enrollment continues to grow.
Related: Justice And Privacy For All: Healthcare Fight For The LGBTQ+ Community Rages On
Florida has enacted the most sweeping changes so far. In March, the state implemented new rules that dramatically reduced eligibility for its ADAP program. Previously, people earning up to 400 percent of the federal poverty level qualified for assistance. Under the new policy, the threshold has dropped to 130 percent of the federal poverty level. The change is expected to cut off benefits for roughly 16,000 Floridians living with HIV.
Advocacy groups report that patients are already feeling the effects of the changes. Some are attempting to ration their medication or share pills in order to stretch remaining supplies.
“Ending the HIV epidemic in the United States requires major investment from our federal government in HIV prevention, treatment, and support services in every state, county, and city in the country,” said Carl Baloney, Jr., President and CEO of AIDS United, in a press release.
“These investments prevent transmission, keep communities safe, save money over time by avoiding more expensive care later, and save lives,” Baloney continued. “Each HIV infection prevented saves an estimated half-million dollars in lifetime treatment costs. Cutting public health infrastructure now is cutting our future.”